Alternative to animal experiments
Teaching a chip to see
Organ-on-a-chip technology has the potential to revolutionize drug development. Researchers at the Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB have succeeded in putting various types of tissue onto chips. Their latest coup has been to recreate the human retina in the form of a retinal organoid. In a parallel development, the research team hopes that organ-on-a-chip technology will open up the field of gender-specific medicine.
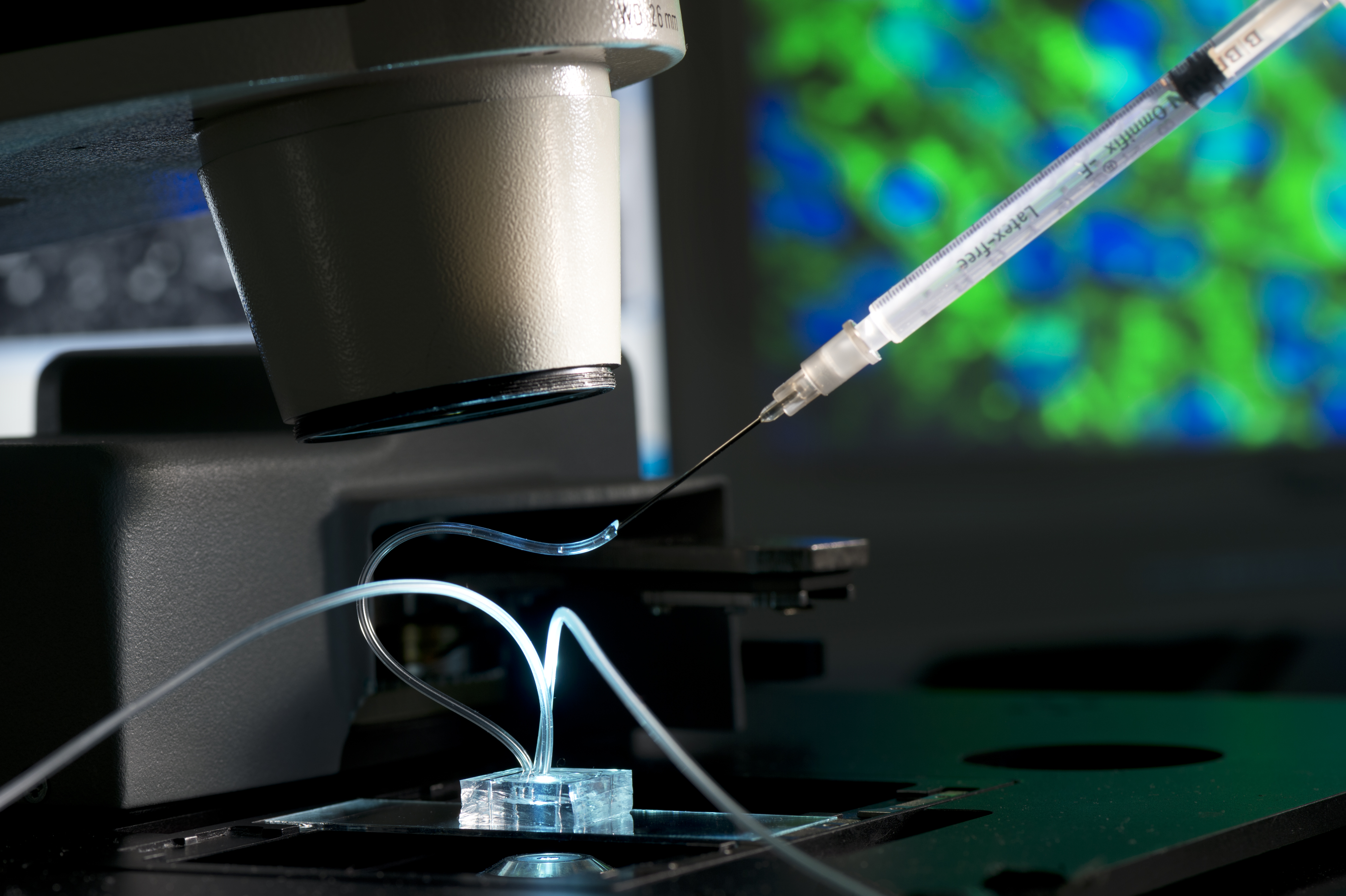

The development of organ-on-a-chip technology marks a huge advance for medical research and now offers a genuine alternative to animal experimentation (see interview below). An OOC comprises polymer chambers the size of a postage stamp, in which minuscule tissue cultures and organoids are fed with nutrients via a system of microchannels. Researchers use these live cultures to test active ingredients, investigate the etiology of diseases and research new drug therapies.
In recent times, OOC systems have been developed for a broad range of tissue types, such as cardiac muscle, liver, kidney and even brain tissue. Helping to spearhead European research in this field is the working group headed by Prof. Peter Loskill at the Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB in Stuttgart. Loskill’s team has pioneered a number of unique developments, including the recreation of white adipose tissue and human retinal tissue on a chip. Now that scientists have mastered the technique of placing a whole variety of tissue cultures on a chip, the next challenge is to accelerate throughput of the various substances being tested. So-called organ-on-a-disk systems will combine hundreds of human tissue samples in one handy format, thereby helping to turn this technology into a routine procedure.
Retina-on-a-chip
The latest breakthrough to emerge from Loskill’s lab is a retina-on-a-chip system, featuring the complex stratified tissue of the human retina as an organoid. Right now, Dr. Loskill and his team are busy endowing their retina-on-a-chip with the capacity to see. Working with partners from the University of Tübingen, they have been able to differentiate stem cells and incorporate them in a chip in such a way that they recreate a multilayer tissue. This tissue comprises, among other things, light-sensitive rods and cones, retinal pigment epithelium and ganglion cells, which make up the optic nerve. “When we shine light on the retina-on-a-chip, we register an electrophysical signal in the rods and cones,” Loskill explains. “And now we’re working on a system with which we can quantitatively measure these signals.”
Researching diseases of the retina
Such a system will make it possible to measure the extent to which a substance influences the “visual capacity” of the retina-on-a-chip. “The pharmaceutical industry is showing a big interest in retina-on-a-chip technology,” Loskill adds. “Lots of modern drugs have retinopathic side effects.” Model systems are still rare in this field, apart from animal models, which are only of limited use, since the retina of the animals used in this field of research has a different structure to that of the human retina. In addition, retina-on-a-chip technology will also facilitate research into diseases of the retina and the development of drugs to treat conditions such as age-related macular degeneration and diabetic retinopathy.
Deciphering the role of fatty tissue
Of even greater medical significance are so-called WAT-on-a-chip systems. WAT is the abbreviation for white adipose tissue – a key factor in human health, not least because it makes up such a significant proportion of body mass. Adipose tissue comprises a quarter of the body mass of a healthy person and up to half the body mass of a clinically obese person. It has only recently become clear that adipose tissue is responsible for secreting a whole variety of hormones and other chemical messengers into the blood stream. Much of this field is still not properly understood, but WAT-on-a-chip systems should help deepen our understanding of the role that white adipose tissue plays in the body and enable researchers to develop more selective treatment for associated diseases such as diabetes. In addition, WAT-on-a-chip systems can reveal the processes by which substances are stored in adipose cells and whether herbicides, for example, or microplastics accumulate in fatty tissue.
Research in gender-specific medicine
Loskill also expects organ-on-a-chip technology to open up a further field of research – that of sex-specific medicine. “Many diseases manifest themselves in different ways in male and female patients,” he explains. “It’s an aspect that has not yet received enough attention in medical research and drug development.” In the future, organ-on-a-chip systems will enable researchers to investigate male or female tissue separately. For example, a female organ-on-a-chip system could be used to simulate the menstrual cycle and observe whether it has an impact on a specific disease and potential drug therapies.
Interview
Dr. Loskill, will organ-on-a-chip technology help reduce large-scale animal experimentation?
Loskill: For sure. We’re already seeing a big interest on the part of the pharmaceutical industry. The technology can be used right across the board: screening for new active ingredients, carrying out toxicity tests and backing up clinical studies.
Will the regulatory authorities accept organ-on-a-chip data in place of results from animal experiments?
Loskill: The regulatory authorities are very open to the technology. I’m currently working on two EU projects involving several agencies, including the German Federal Institute for Drugs and Medical Devices (BfArM).
In the long term, will your technology make animal experiments completely redundant?
Loskill: No technology alone will ever be able to completely replace animal experimentation. But our chips do provide a source of data that will enable us to gain requisite certainty with significantly fewer animal experiments.
 Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB
Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB