Production line for artificial skin
A fully automated process is set to improve the production of artificial tissue: medical scientists can perform transplants with skin produced in the laboratory. This tissue is also suitable for testing chemicals at a low cost without requiring animal experiments.
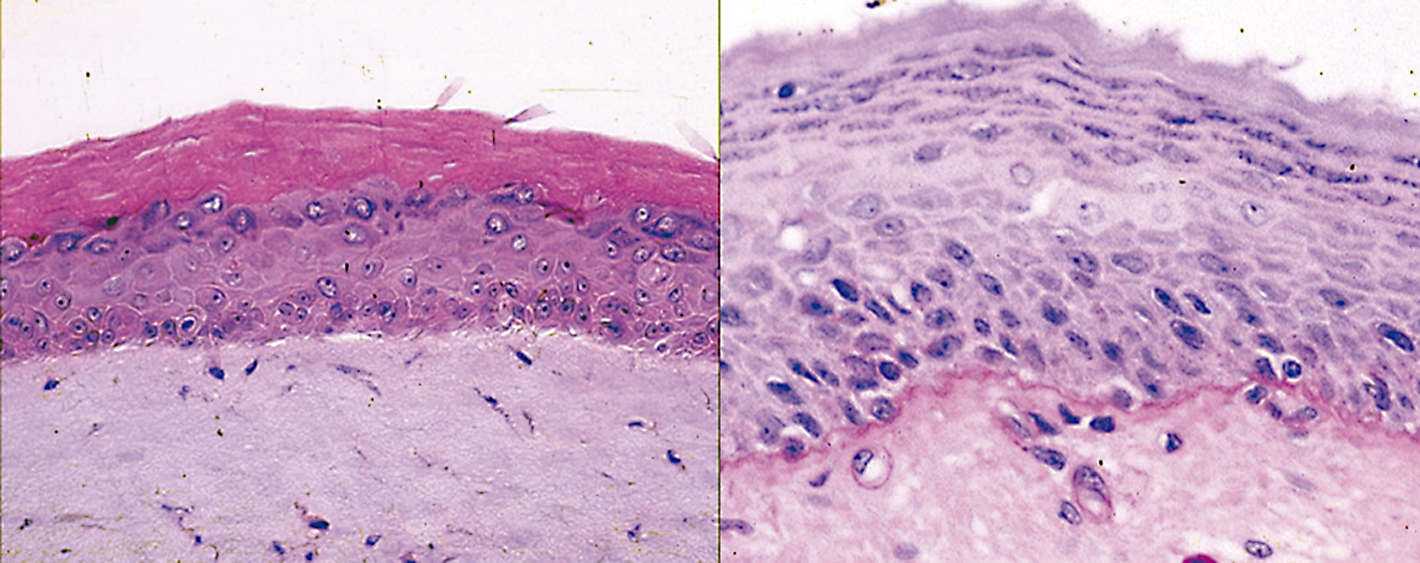
Some patients wish they had a second skin – for instance because their own skin has been burnt in a severe accident. But transplanting skin is a painstaking task, and a transplant that has to cover large areas often requires several operations. Medical scientists have therefore been trying for a long time to grow artificial tissue. This “artificial skin” would allow them to treat these patients better and faster.
Tissue engineering has been at the focus of research for many years, and tissues such as cartilage or skin are already being cultured in numerous biotechnology laboratories. But the researchers at the Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB in Stuttgart plan to go a step further than that. They are aiming to enable fully automated tissue production. “Until now, methods of culturing tissue like that used for skin transplants have been very expensive,” says IGB head of department Professor Heike Walles. “Most of the steps are carried out manually, which means that the process is not particularly efficient.” The researchers have therefore elaborated a novel conceptual design in collaboration with colleagues from the Fraunhofer Institutes for Production Technology IPT, Manufacturing Engineering and Automation IPA, and Cell Therapy and Immunology IZI.
First of all, a biopsy – that is, a sample of human tissue – is checked for sterility. A gripper arm then transports the biopsy into the automated device where the individual steps are performed: The machine cuts the biopsy into small pieces, isolates the different cell types, stimulates their growth, and mixes the skin cells with collagen. A three-dimensional reconstruction of the different skin layers is produced with the aid of a special gel matrix – and the skin is ready. In the final step, the machine packages the cells for shipment. Alternatively, the tissue can be cryopreserved – that is, deep-frozen and stored for later use. “It was important for us that the entire mechanical process is divided into separate modules,” says Walles. “This enables us to replace or modify individual modules, depending what is needed for the production of different tissue types.” The method opens up almost unlimited new possibilities for the medical scientists. One of their upcoming projects is to produce intestinal tissue for resorption tests.
 Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB
Fraunhofer Institute for Interfacial Engineering and Biotechnology IGB